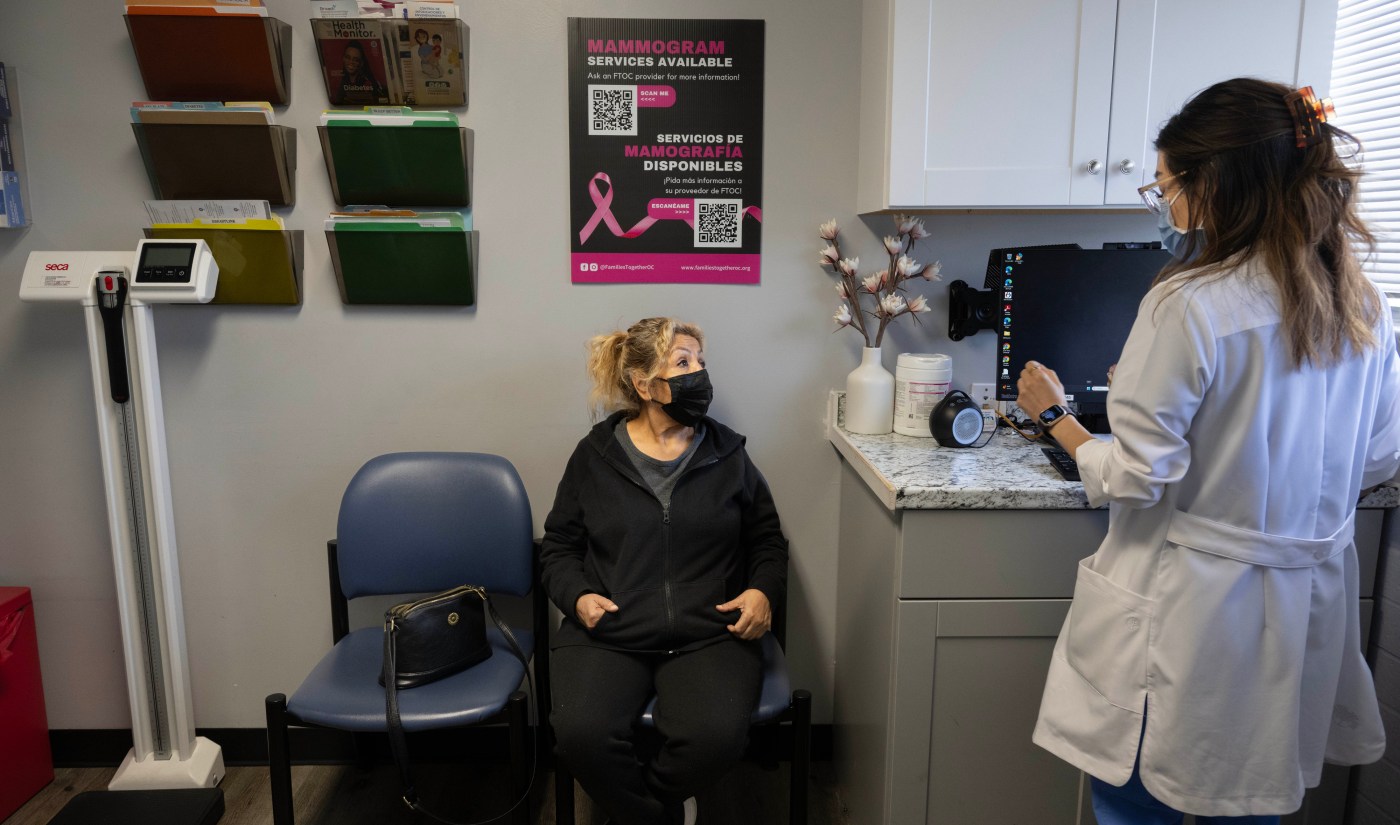
CalOptima, Orange County’s health insurance program for the poor, has seen a plunge in membership since summer, which advocates attribute to the effects of the Trump administration’s hardline immigration policies and sweeping changes to Medi-Cal.
More than 26,500 CalOptima members have left since the start of the year, dropping the total enrollment to roughly 822,000 in mid-February, according to data shared by the agency. Some 15,000 people dropped from the health plan just in February.
Yunkyung Kim, CalOptima’s chief operating officer, said enrollment numbers are now “far below” the agency’s projections for the year.
There has been a consistent decline since July, officials said, when nearly 886,000 people were enrolled with CalOptima, which serves about one-third of the county’s population.
California had expanded Medi-Cal coverage in 2024 to undocumented adults, becoming one of the first states to offer health care to low-income residents regardless of immigration status. An estimated 700,000 people enrolled.
The state’s Medicaid program covers more than 15 million lower-income residents, including 1.7 million undocumented immigrants.
In July, it was reported that the Trump administration gave U.S. Immigration and Customs Enforcement agents access to the personal data of 79 million people enrolled in Medicaid. The data-sharing agreement, signed between the Centers for Medicare and Medicaid Services and the Department of Homeland Security, was intended to help the agency track down undocumented immigrants.
President Donald Trump has supported mass deportations of undocumented immigrants as part of his promise to expel violent criminals, better secure the country’s borders and to put Americans first.
“Since last summer, we’ve heard a lot of anxiety in the community about the impact of data sharing on immigration status and future immigration opportunities,” Kim said. “We weren’t really surprised when we saw the hesitation to keeping medical insurance.”
Also affecting enrollment have been cuts to Medi-Cal stemming from Trump’s massive tax and spending bill last year, House Resolution 1, also known as the One Big Beautiful Bill Act. And, California’s $321 billion budget for the current fiscal year also established limits for residents without permanent legal status.
As a result of the funding shortfalls, the state froze new enrollment of undocumented Californian adults ages 19 and older, starting Jan. 1. The 1.6 million undocumented residents currently enrolled in the program were not ejected, but they cannot re-enroll if they lose coverage. After July 1, 2027, they’ll be required to pay $30 a month to maintain full coverage.
Children 18 and younger and pregnant people can continue to enroll in the program regardless of their immigration status.
Starting in 2027, individuals between the ages of 19 and 64, regardless of citizenship status, will be required to work or volunteer for at least 80 hours a month to stay enrolled in Medi-Cal.
Around 3 million Californians are projected to lose Medi-Cal coverage by 2028 as a result of policy changes from HR 1 and the state budget, according to a new report from the UCLA Center for Health Policy Research and the UC Berkeley Labor Center. Roughly 250,000 Orange County residents are projected to lose coverage in the next two years.
Kim said the freeze in Medi-Cal eligibility that went into effect Jan. 1 impacted only a small portion of the population. Also, some people had already lost coverage late last year during the annual redetermination process, Kim said, typically due to paperwork issues or life changes.
“Sometimes, your circumstances change and you don’t need Medi-Cal anymore, and hopefully that means you have another source of coverage,” Kim said. “But there is anxiety in the community about how future policy decisions will impact families. So we can’t discount that there are some decisions being made at individual or family levels about whether to continue to pursue Medi-Cal coverage.”
CalOptima, in the meantime, has invested significant resources into educating members about the renewal process and onslaught of new requirements, Kim said. The health plan launched a $20 million initiative last October, engaging local media outlets, social media, newsletters and community organizations to guide members through the labyrinth of eligibility and enrollment changes to Medi-Cal.
Those who are no longer eligible for Medi-Cal can look for plans on Covered California, Kim said, which is more affordable than buying health insurance on the open market. Kim said CalOptima is working on bringing a new Covered California plan to Orange County residents next year.
More people not receiving Medi-Cal coverage means that tens of thousands of residents will likely end up relying on community clinics and emergency room care, advocates say.
“Community health centers are often the first place people turn when they lose coverage, and we do anticipate increased demand for services as more patients become uninsured,” said Alexander Rossel, the CEO of Families Together of Orange County, which operates two low-cost health clinics in Tustin and Garden Grove.
An influx in uninsured patients, Rossel said, may force clinics to “make difficult decisions” about how to allocate available resources, which can affect the clinics’ staffing, appointment availability and range of services that providers can offer. The health center may also need to reassess whether it can maintain wraparound services such as transportation assistance and food pantry support, he said.
Rossel said access to community-based primary care plays an important role in reducing strain on hospitals and emergency departments across the county. About three-quarters of patients at Families Together rely on Medi-Cal, while 10% are uninsured. The clinic does not inquire about the immigration status of patients it serves.
At AltaMed Health Services, which has clinics throughout Los Angeles and Orange counties, about two-thirds of patients rely on Medi-Cal, said Kimberly Graham, director of patient access. The clinics serve undocumented and uninsured patients, who have the option of paying on a sliding scale depending on their income level.
Graham said AltaMed, like CalOptima, has launched a multimedia campaign to inform community members about the forthcoming Medi-Cal changes so that they don’t lose coverage.
“Our foot is on the gas as related to patient education,” she said. “We did a robust marketing campaign via television ads, social media, phone and in-clinic and community events.”